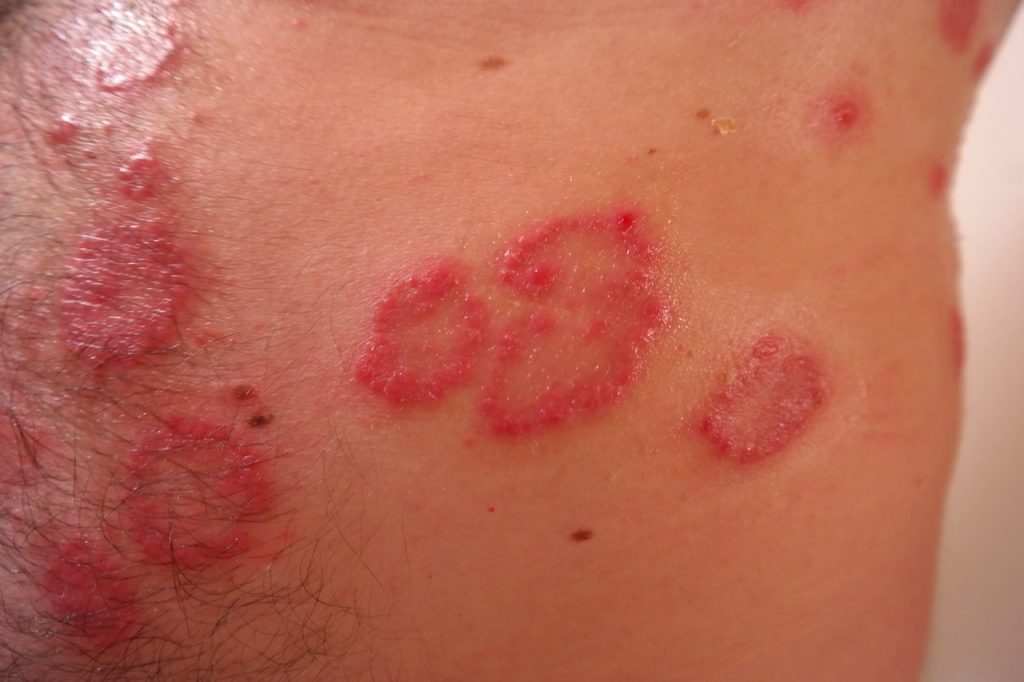
What is diabetic dermopathy?
Diabetic dermopathy is a relatively common skin problem for people living with diabetes. The condition does not occur in everyone with diabetes. However, it is estimated that around 40-50 percent of individuals living with the disorder will develop some kind of skin disease, such as diabetic dermopathy.
Diabetic dermopathy condition causes small lesions on your skin, such as an abnormal lump, bump, ulcer, sore, or colored area. They are sometimes reddish or brown and are usually round or oval. Diabetic dermopathy typically appears as dull red or brown scaly patches on the shins which don’t sting or itch. According to different sources, it may affect more than half of all people with diabetes. Doctors do not know what causes it exactly, but it tends to appear in people who have diabetic neuropathy or blood vessel complications or have had diabetes for a long time.
Lesions can appear anywhere on your body, but they tend to develop on bony parts. It’s typical for them to grow in your shins. Diabetic dermopathy is sometimes known as shin stains or pigmented pretibial patches.
See: Milk for diabetics
Other common skin manifestations in diabetics are:
– Diseases: Pyogenic (Staphylococcal), Fungal (candidiasis, etc.)
– Other Dermatoses: Xanthomas, Neuropathic foot ulcers, and sclerodactyly.
– Candida Infections: Candidal skin ailments are more recurrent and extensive in diabetes, especially in undiagnosed diabetics, e.g., candidal vulvovaginitis and skin folds (groins, interdigital, intramammary, prepuce) and nails (Paronychia).
– Necrobiosis Lipoidica: It generally affects young girls with type-1 diabetes. It’s present in single or multiple asymptomatic hardened, annular, yellow-brown plaques and typically involves pretibial area and shins.
– Granuloma Annulare: These are generalized or localized red plaques on the limbs or trunk of the body.
– Scleroderma: These will be the regions of skin thickening on the trunk and neck at the website of prior superficial infections in diabetics.
– Neuropathic Foot Ulcers: They generally result from poor blood flow, infections, and poor hygiene care.
– Sclerodactyl: it’s the hardening of the skin of the fingers and feet in diabetic patients.
– Pyodermas: Pus forming eruptions on the skin brought on by a staphylococcus group of germs. Infection to hair follicles (furunculosis, folliculitis) and carbuncles are widespread manifestations among them.
– Diabetic dermopathy: Commonly known as “Diabetic skin stains.” It begins as a red area over the skin and evolves into superficial hyperpigmentation after the shedding of scales. These are more common in older diabetics.
– Acanthosis Nigricans: It is normal in obese and insulin-resistant diabetics. These exist in the kind of velvety hyperpigmented plaques in axillae, inguinal area, and intramammary folds.
What causes diabetic dermopathy?
Diabetic dermopathy causes:
Despite the fact that diabetic dermopathy is common once you’re living with diabetes, this problem’s specific cause is unknown. However, there is a theory about the underlying mechanism behind those stains. Shin spots are connected to leg injuries, leaving some physicians to conclude that the lesions may be an exaggerated reaction to injury in people who have diabetes that is not well-managed.
Uncontrolled diabetes often results in poor circulation or insufficient blood circulation to different body areas. Over time, poor circulation can decrease the body’s wound-healing abilities. Reduced blood flow to the area surrounding an injury prevents a wound from healing correctly, leading to the evolution of bruise-like spots or lesions.
It seems that nerve and blood vessel damage resulting from diabetes may also predispose one to diabetic dermopathy.
This illness has been associated with diabetic retinopathy (eye damage), diabetic nephropathy (kidney damage), and diabetic neuropathy (nerve damage). Additionally, it appears to be more prevalent in men, elderly adults, and those who have had diabetes for a more extended period. There is no available research to verify this information. It is just a theory about what causes diabetic dermopathy.
See: Ramadan & Suhoor Diet For Diabetics
Diabetic dermopathy symptoms
What are diabetic dermopathy symptoms?
The look of diabetic dermopathy can differ from one person to another. The skin is characterized by reddish-brown marks and round or oval with scar-like stains. It is typically asymptomatic, meaning it generally does not present any symptoms. Lesions primarily form on the shins, but they may be found in other areas of the body, too. However, they’re not as likely to develop in these areas.
Diabetic dermopathy does not usually cause symptoms such as burning, burning, or itching. You may develop one lesion or clusters of lesions on the shin and other parts of your body. When spots develop on the body, they frequently form bilaterally, meaning that they occur on both legs or arms. Aside from the appearance of skin lesions, diabetic dermopathy does not have any other symptoms. These lesions or patches do not break open or discharge fluids. They are also not contagious.
Your physician might have the ability to diagnose diabetic dermopathy following a visual exam. If your physician decides you have diabetic dermopathy, they can forgo a biopsy. A biopsy may pose concerns about slow wound-healing. However, you might require a skin biopsy if your physician suspects another skin condition.
Diabetic dermopathy may be an early symptom of diabetes. You may experience other early signs of getting diabetes. These include blurry vision, weight loss, frequent urination, frequent thirst, fatigue, and tingling sensation in your limbs.
When you haven’t been diagnosed with diabetes, and your physician concludes your skin lesions may be due to diabetic dermopathy, they may order additional tests. The evaluation results will help them confirm your diagnosis.
Ayurvedic diabetic dermopathy remedies
Ayurvedic remedies for diabetic dermopathy
Skin is the broadest and vertical system of the human body. It’s in ultimate contact with the outside environment. Any chemical or physical change in the external or internal environment (body) directly affects the skin and its appendages such as hairs, sweat glands, nails, etc. and many times, it provides a hint to a lot of internal diseases like Diabetes & Renal disorders. Diabetes mellitus, commonly called Madhumeha in Ayurveda. Lots of uncontrolled or poorly controlled diabetic patients suffer from skin ailments.
Taking care of diabetic dermopathy
Diabetic dermopathy is benign and does not necessarily require treatment. Blood glucose control can be helpful for slowing the development of diabetic neuropathy and cardiovascular disease that often goes with it. There is no specific treatment for diabetic dermopathy. Some lesions may take weeks to fix, while others might take over a year. There are other cases where lesions could be permanent. You can not control the speed that lesions fade, but you can take steps to deal with the condition. Listed below are a few management tips:
– Moisturizing can also help enhance the appearance of stains.
– Applying makeup might help cover the stains.
While there is no specific diabetic dermopathy treatment, managing your diabetes remains important to stop diabetes-related complications. No comprehensive remedy for diabetes has been demonstrated so far, and complications of uncontrolled diabetes are more severe than the disease itself. But we can keep it in check with appropriate diet, exercise, and medications if needed.
– Manage high blood sugar levels.
– Ayurvedic Massage: Approaches to improve subcutaneous blood flow should be implied, e.g., massage, skincare packs, patting, etc..
– General body health ought to be maintained with the support of mild exercises, Yogasanas (Dhanurasana, Ardha-matsyendrasana, Sarvangasana, Halasana, Yogamudrasana, Bhujangasana,Chakrasana etc..)
– Medicines: Diabetic patient has to maintain regular contact with their doctor and take normal medications prescribed by him.
– Regular blood glucose level monitoring. Check the higher blood sugar level and to keep it with the support of oral hypoglycemic agents (e.g., Sulfonylureas, Biguanides) and nourishment.
– Treat skin ailments, appropriate antifungal, and antibacterial agents should be used (oral or local use or both if necessary).
– Natural herbal remedies: Shilajeet, Haridra, Guduchi, Nimb, Vijaisar, Gudmar, Methi, Karela, Triphala, Ashwagandha, Phaltrikadi kwatha, Lodhrasava, Madhvasava, Shiva gutka, Chandraprabhavati, Basantkusumakar ras are beneficial to assess and to counteract the side effects and complications. These medications also restore overall health and boost the immunity of the patient.
Summary
Diabetic dermopathy is a frequent illness in people living with diabetes. The problem is characterized by the presence of lesions. These lesions are benign and do not cause any pain, but they should not be ignored. You must keep your diabetes well-managed, which entails regularly monitoring your blood glucose. Handling your condition is important in preventing further diabetes-related complications such as the increased risk of stroke or heart attack, or nerve damage.
Schedule regular visits with your physician to go over your diabetes treatment plan and modify your diet and lifestyle to keep good glycemic management. For instance, if you take your medicine as prescribed, but your blood glucose stays high, speak with your physician. You might need to adjust your existing therapy. Make a concerted effort to work out three to five times weekly. Routine exercise is vital to your general health. This exercise can include walking, biking, or swimming. Eat fresh fruits, vegetables, and lean meats. It’s crucial to consume a healthy, well-balanced diet. Losing weight can help stabilize your blood sugar level if you are overweight. It is essential to protect your shins and thighs because diabetic dermopathy tends to mostly affect these regions. Scheduling regular visits with your health care provider will allow them to complete a comprehensive examination to help determine the best management plan for your problem. Diabetes control entails maintaining healthy blood glucose, reducing stress, and quitting smoking.