What is Ulcerative Colitis?
What is Ulcerative Colitis?
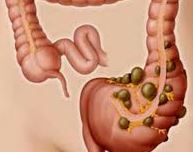
Ulcerative Colitis is irritation (inflammation) of the large intestine’s internal lining, also called colon (part of the gut in which water is reabsorbed and waste materials such as excretion) are stored briefly. It also involves the lining of the anus.
This inflammation leads to ulceration or swelling, which could contribute to painful bowel movements, bloody diarrhea (bloody stools), and rectal bleeding. This disorder is medically grouped under Inflammatory bowel Disease or IBD. The lesions in ulcerative Colitis primarily involve the anus and might spread to the sigmoid colon. In rare circumstances, the whole colon can be involved in a condition called pancolitis. Ulcerative Colitis can have alternating periods of flare-ups and remission.
It is found worldwide but is most frequent in the USA, England, and northern Europe. It’s particularly common in people of Jewish descent. Ulcerative Colitis is seldom seen in Eastern Europe, Asia, and South America, and is uncommon in the black population. For unknown reasons, an increased frequency of the condition was observed recently in developing nations. It may also indicate an industrial or Western diet, and lifestyle increases the incidence of this disease Ulcerative Colitis can be intermittent from symptom-free periods to exacerbated symptoms.
In patients with Ulcerative Colitis, the immune system is abnormally and chronically activated in the absence of any known invader. The continuing abnormal activation of the immune system causes chronic inflammation and ulceration.
It is an autoimmune disease in which the body resistance cells are fighting against your body cells –causing damage to the lining of the colon and rectum and changing its role producing abnormal symptoms such as bloody diarrhea and painful defecation. It causes general distress in the individual where day to day activities of the person gets affected.
See: Ginger for acid reflux relief
Symptoms & Causes of UC
Reasons For Ulcerative Colitis
Ulcerative Colitis starts most commonly during adolescence and early adulthood, but they can also begin during childhood and later in life. Factors believed to be responsible include:
– Environmental
– Genetic
Diet: A High intake of unsaturated fat and vitamin B6 can increase the risk of developing UC.
– A diet containing a high amount of sulfur
– Patients with milk allergy
– Attacks have been flared up by high protein meat and alcohol
– Recent studies have shown that people with a higher level of emotional and stressful life events, such as death or divorce, have proven to precipitate the disease.
Symptoms of Ulcerative Colitis
Owing to the autoimmune nature –the signs aren’t merely limited to colon and rectum. Due to the intrusion of immunity cells in different areas of the body, symptoms are expressed there, combined with main symptoms.
– Patients usually present with diarrhea combined with mucus and blood, of slow-onset that persists for a protracted period (months).
– Mild to function painful bowel movements
– Crampy pain in the gut when passing stools
– Blood loss
– Weight reduction
– Extraintestinal Characteristics: Patients with ulcerative Colitis can sometimes have aphthous ulcers involving the tongue, lips, palate, and pharynx.
– Clubbing: deformity at the end of the palms
– Inflammations of the veins –swelling of the veins –resulting in thrombosis
– Eyes: Redness of eyes
– Joints: inflammations of joints called arthritis especially backbone –swelling and pain of the joints
– Skin: redness and nodosities
If Ulcerative Colitis is suspected based on clinical symptoms, additional laboratory tests are advised. These can include colonoscopy, biopsies, and sigmoidoscopy, and of the mucosa removed in the colon. A biopsy, while helping the diagnosis of ulcerative Colitis, also helps distinguish it from Crohn’s disease. The ideal test for the diagnosis of ulcerative Colitis remains sigmoidoscopy to determine the inner nature of the lining of the colon and the anus.
Blood in feces is a significant sign of ulcerative Colitis. However, blood in feces can also be noted in other conditions like hemorrhoids (piles), anal fissures, and peptic ulcers. Further investigation concerning stool examination, endoscopy, sigmoidoscopy, and colonoscopy must be conducted before the precise cause could be established.
Homeopathy medicines for Ulcerative Colitis
Homeopathy Treatment for Ulcerative Colitis
All autoimmune diseases are linked to stress. Homeopathy helps to boost the immune system of the body. Modern medicine can only take care of the symptoms of this disease but not the root cause. Hence the effect is only temporary with possible side effects. Homeopathic medicines treat the mind and its influence on the body at the same time. Homeopathy may improve the symptoms and quality of life over time and may induce remissions over some time with continued therapy.
Homeopathy Medicines for Ulcerative Colitis
Some well-recognized medications for Ulcerative Colitis are Merc Sol, Merc Cor, Colchicum Autumnale, Aloe Socotrina, and Phosphorus, Silicea, Phosphorus, Terebenthina, Mercurius, Arsenic, Alumina, Sulphur, Thuja, and Nitric acid.
Homeopathy medicine is a trusted alternative to modern medication in treating autoimmune disorders, including ulcerative Colitis. Homeopathic medicines for ulcerative Colitis moderate the overactive immune system. The area of improvement and advantage will depend on a high number of factors such as the length and intensity (mild/moderate/severity) of disease, the stage where Homeopathy medicines are started, and individual body reaction.
Homeopathic medications for ulcerative Colitis can help manage symptoms, decrease the frequency and severity of flare-ups, and treat Ulcerative Colitis based on individual case analysis.
– Colchicum Autumnale: Colchicum Autumnale is another medication for ulcerative Colitis where joint pains appear together with gastric symptoms. The pain in anus lasts for a long time after the stool is passed. Highly offensive flatus may attend the symptoms mentioned above. In terms of the joint pains, the joints may be swollen, stiff, and in sharp pain.
– Merc Cor: Merc Cor is a suitable medicine for Ulcerative Colitis with loose stool, mucus, and blood. The stool is offensive and hot. There may be a sensation of burning in the rectum when passing stool may emerge. There can be cutting, colicky pains in the gut also.
– Phosphorus : Phosphorus is a considerable medication for treating ulcerative colitis cases with bloody diarrhea attended with fatigue. The individual feels tired after passing stool. Cramping pain in the anus may emerge on passing stool. The blood is bright red.
– Merc Sol: Merc Sol is one of the best grade medications for ulcerative Colitis and is best suggested for cases of loose stools with excessive bleeding. The stools are extremely frequent. But even after passing stool lots of times, there’s not any satisfaction. Such persons often feel cold all the time.
– Nux Vomica: Nux Vomica is a most useful medication for ulcerative Colitis with frequent, scanty stool and conspicuous tenesmus (the ineffectual urge to pass stool nearly always). The stool is tiny. Abdomen pain before passing feces might be observed. Nux Vomica also provides great help in cases where taking hot food or alcohol worsens symptoms.
– Aloe Socotrina: Aloe Socotrina is suitable for ulcerative Colitis with urgency to pass stool as the predominant symptom. The necessity to pass stool is present in the morning, also shortly after eating or drinking. There’s constant bearing down in the anus. Burning from the rectum and anus may also be intense. Aloe Socotrina is also suited for the passing of jelly-like mucus in feces.
– Nitric Acid: Nitric Acid is the ideal choice of medication in ulcerative colitis cases where there is intense pain in the anus when passing stool. The pain could be tearing or cutting in nature. It could last for hours after the stool is passed. Profuse, bright red bleeding might be noticed alongside stool in such instances.
– Lifestyle changes help to better handle ulcerative Colitis: Reducing stress levels and dietary changes can have a positive impact on UC. Ayurvedic diet, massage meditation, exercise, yoga class, or take regular walks to bring down stress and remain calm. Avoid alcohol, caffeine, dairy products, spicy foods, and a higher fiber diet.
Complications: Ulcerative Colitis may result in complications. These include perforation of the colon, osteoporosis, severe bleeding, joint inflammation, eye inflammation, colon cancer, and toxic megacolon.
Can Homeopathy Treatment adequately treat UC? Homeopathy medications can be effective in treating ulcerative Colitis. Recovery and healing can vary based on a person’s constitution, genetics, and many other factors.
See: Home Remedies for Heartburn
Make diet a priority with Ulcerative Colitis
UC can affect your body’s ability to:
– Properly digest food
– Absorb nutrients
These breakdowns in the digestion process may result in serious vitamin deficiencies and deficiencies. When it comes to your diet, be sure you include enough calories and nutrients to keep you healthy–reducing your risk of malnourishment. Work with the healthcare team that will assist you in maintaining adequate nutrition. Make nutritious food choices–and avoid foods that could make your symptoms worse.
What Causes Malnutrition With UC?
Frequent symptoms of UC can result in malnutrition–along with intestinal inflammation. Symptoms like:
– Severe diarrhea may cause dehydration
– Frequent bowel movements might induce you to reduce eating to Prevent nausea
– Abdominal pain and nausea can reduce your appetite
– Bleeding from ulcers can lead to anemia or iron deficiencies
See: North Indian Diet plan for High Uric acid levels and Gout
Tips on Food and Symptom Flares
While there is no evidence that what you eat causes UC, certain foods and beverages can aggravate your symptoms–particularly during a flare-up. Keep track of what you are eating and how you feel to help you find some foods that may exacerbate your symptoms. Some tips to figuring out how foods might affect you include:
– Try low-fat foods
– Restrict fiber (if it is a problem food)
– Limit dairy
– Avoid spicy foods, alcohol, and caffeine.
And here are some other dietary steps to consider when ensuring you are getting the nutrients you need:
– Eat smaller meals, more often, rather than the regular 2-3 larger ones per day
– Drink plenty of liquids
– Keep hydrated
– Consider multivitamins
– Speak with a registered dietitian