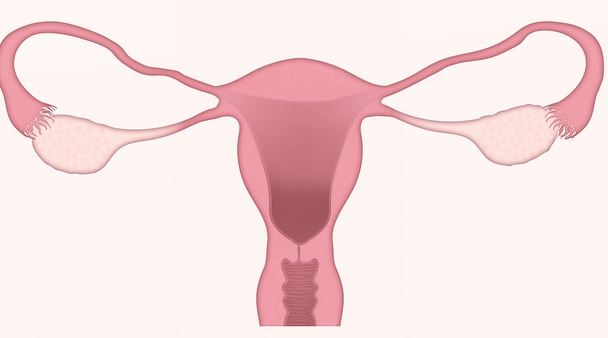
PCOS is a complex metabolic disorder and requires an integrative approach. PCOS natural treatment & home remedies include dietary changes, yoga & detox programs to lower stress. PCOS treatment in Ayurveda includes a combination of herbs, customized therapies, and lifestyle changes, such as yoga, meditation, and diet.
What is PCOS?
Polycystic ovary syndrome (PCOS) is a complex hormonal disorder. Women can manage PCOS symptoms at home with healthy diets, yoga, exercises, dietary supplements, and other home remedies for PCOS. You can fight the adverse effects of hormonal changes by increasing your insulin resistance and stamina. Because PCOS symptoms can overlap with other diseases, a woman experiencing them should seek medical advice from a gynecologist. PCOS may also be linked to diabetes, heart disease, high blood pressure, obesity, high cholesterol, and metabolic syndrome. PCOS is a gynecological disorder whose prevalence seems to have increased considerably in the last few years. Many young girls and middle-aged women suffer from this syndrome, marked by the appearance of multiple cysts on ovaries and disturbances in monthly menstrual cycles.
See: Yoga Asanas For Healing PCOS
Polycystic ovary syndrome (PCOS) happens when a female’s ovaries or adrenal glands produce more male hormones compared to normal. It’s considered a hormonal disorder and is not uncommon among women of reproductive age. Women with PCOS may have rare or prolonged menstrual cycles or excess male hormone (androgen) levels. The ovaries may develop numerous little collections of fluid (follicles) and fail to release eggs frequently. The exact cause of PCOS is unknown. Early diagnosis, treatment, and weight loss may decrease the risk of long-term complications such as type 2 diabetes and cardiovascular disease.
There is no cure, but exercise, diet, and lifestyle modifications can help control the symptoms.
See: Naturopathic Medicine Treatment For PCOS
PCOS Symptoms
Signs and symptoms of PCOS often develop around the first menstrual period throughout puberty. Sometimes PCOS develops afterward in response to substantial weight gain.
Symptoms and signs of PCOS vary. Chances you may have PCOS increase if you experience at least two of the following signs:
· Irregular periods. The infrequent, irregular, or prolonged menstrual cycle is the most typical sign of PCOS. By way of example, you might have fewer than nine periods a year, over 35 times between intervals and abnormally heavy periods.
See: Insulin resistance symptoms & diet for PCOS
· Excess androgen. Elevated levels of male hormones might result in physical signals, such as excess facial and body hair (hirsutism), and sometimes severe acne and male-pattern baldness.
· Your ovaries might be enlarged and contain follicles that encircle the eggs.
PCOS signs and symptoms are typically more severe if you’re obese. In this condition, the eggs and follicles are not released from the ovaries but form multiple cysts. Obesity is linked to the condition, as 50 percent of women with PCOS are obese. Hormonal imbalances perform a major role in this condition, such as elevated levels of the hormone androgen and Low levels of progesterone, the female hormone required for egg release. Although PCOS was formerly considered an adult-onset condition, more recent research indicates that it starts in youth, possibly even during fetal development.
See: Ayurvedic herbs to heal PCOS
What causes PCOS?
The root cause of nonfunctional ovarian cysts is not yet completely understood. Many factors are believed to play a role in the growth of cysts, such as a female’s general health, weight, diet, history, and way of life. The mind/body connection might also be a variable with migraines, as high anxiety and stress levels might be notable facets. Some complementary therapy professionals and psychotherapists believe that unexpressed imagination and repressed emotions like guilt and anger might be linked to uterine problems. For PCOS, obesity, hormonal imbalance, and higher blood glucose levels are closely linked to the condition. It has been observed that women with PCOS are five to ten times more likely to develop type 2 diabetes compared to others.
See: Keto diet benefits for weight loss, diabetes & PCOS
PCOS is also known to run in families, which suggests that genetic factors contribute to its development. As of 2002, the particular gene or genes responsible for PCOS haven’t yet been identified; nonetheless, many groups of researchers in various nations have been investigating genetic variations associated with a greater risk of type 2 diabetes in order to ascertain whether the exact same genetic variants may participate in PCOS.
See: PCOS Supplements To Heal Symptoms
Some cysts may be asymptomatic (without symptoms), while others can cause swelling, aching, sharp pain, and bleeding. Pain from cysts can last from a few minutes to a few days. Other indicators of cysts include late or missed periods, feelings of pressure or weight in the lower stomach, constipation, and problems urinating due to internal stress from cysts. Ruptured cysts can cause severe pain and produce symptoms resembling those of appendicitis, disease, or ectopic pregnancy.
• Sudden sharp pain in the lower abdomen
• Persistent pain on the Ideal side of the abdomen accompanied by sickness, fever, or vomiting
• Abdominal pain along with vaginal discharge, fever, or swelling
• Intermittent drops of pain in the lower abdomen during sexual activity, bowel movements, or exercise. [3]
It is now well established that PCOS represents a complex trait similar to type-2 obesity and diabetes and that both inherited and environmental factors contribute to PCOS pathogenesis. According to a 2009 study, although the role of hereditary factors in PCOS is firmly supported, the genes involved in the syndrome’s etiology have never been fully researched until now, in addition to the environmental involvement in their expression. [4]
See: Balance your hormones with Ayurveda
Since PCOS is mostly a genetic illness, the risk of PCOS In household members is large. For example, an estimated 30 percent of moms and 50 percent of sisters and daughters of individuals with PCOS may be impacted. According to 2016 research, the genetics of PCOS remains not fully understood, and early identification and treatment can prevent long-term consequences. In that study, the research team analyzed the proteins involved in PCOS as well as the structural areas of the proteins using modern computational tools. [5]
To date, there is absolutely no cure for PCOS. Healthcare professionals can usually address the most bothersome symptoms. Because of the complexity of hormonal interactions, a trip to a holistic therapy expert may be needed, especially if you are infertile and trying to conceive. [6]
See: Reduce PMS and balance your hormones
PCOS Natural treatments
PCOS treatment focuses on managing your unique concerns, such as infertility, hirsutism, acne, or obesity. Particular treatment might involve lifestyle changes or medication. Your doctor may recommend weight loss via a low-carb diet and moderate exercise. A modest decrease in your weight – for example, losing 5 percent of your body weight – might enhance your condition.
See: How To Balance Hormones Naturally
Many people have also benefited from Ayurveda, Acupuncture, and herbal therapies for PCOS.
To help decrease the consequences of PCOS, these natural therapies with diet, exercise, and lifestyle change therapies can help:
Weight reduction
Losing weight through exercise and healthy eating might help someone reduce PCOS symptoms.
Maintaining a healthy weight is an important part of controlling PCOS symptoms. Individuals with PCOS commonly carry additional weight, which can raise their risk of diabetes, heart disease, and other issues connected with metabolic syndrome. Losing 5-10 percent of body weight might help alleviate PCOS symptoms. Certain lifestyle changes, like eating a balanced diet of healthy foods and getting more physical activity, can assist with weight loss and lower the risk of health complications.
See: Balance Your Hormones With Foods & Herbs
Dietary changes
Changing the diet is a vital part of managing PCOS. Individuals with PCOS often have higher insulin levels, a hormone the body uses to reduce high blood glucose. If the body has persistently elevated insulin levels, it may stop responding to the hormone. Because of this, blood glucose levels may stay elevated. Insulin resistance, a precursor to diabetes, is quite common in people with PCOS, making maintaining a healthy weight hard. Insulin and blood glucose levels increase the highest after someone eats foods full of carbohydrates and/or sugar.
Eliminating simple carbs and sugar in the diet can help stabilize blood glucose and keep insulin levels low. This may mean avoiding white bread, pasta, and rice products. Unlike simple carbohydrates, complex carbohydrates contain fiber and other nutrients and don’t raise glucose levels as high. Some common sources of complex carbohydrates include whole-wheat bread, brown rice, and brown pasta.
Balance protein and vitamin intake
Carbohydrates and protein both affect your hormone and energy levels. Eating protein arouses your body to produce insulin. Unprocessed, high-carb foods can improve insulin sensitivity. Rather than looking for a low-carb diet, concentrate on getting enough healthful protein. Plant-based protein resources, such as nuts, legumes, and whole grains, are best.
Anti-inflammatory diet
PCOS is clarified by one study as low-level chronic inflammation. Adding anti-inflammatory foods to your daily diet can help alleviate your symptoms. The Mediterranean diet can be a good option. Olive oil, tomatoes, leafy greens, fatty fish, and tree nuts help fight inflammation.
Increase your iron & magnesium intake.
Some women with PCOS may have heavy bleeding during their period. This can lead to iron deficiency or anemia. If your doctor has been diagnosed with either illness, talk together about ways to increase your iron intake. They might recommend adding Spicy foods like spinach, eggs, and broccoli.
Almonds, cashews, spinach, and peanuts are PCOS-friendly foods full of magnesium. You should not increase your iron intake without first consulting your physician. Too much iron may increase your risk of complications.
A high-fiber diet can help improve digestion. Broccoli, brussels sprouts, lentils, lima beans, and avocados are full of fiber.
Be active
Exercise helps lower blood glucose levels. In case you have PCOS, increasing your everyday activity and engaging in a regular
exercise program may treat or even prevent insulin resistance and help you
maintain your weight in check and prevent developing diabetes. [2] Exercise is also beneficial for your heart health, and it may enhance your mood, keep a positive mindset, and help regulate sleep patterns. Getting a good workout doesn’t imply working out at the gym. Engaging in some fun physical activity, game, or sport will encourage someone to participate in it consistently and receive the best benefits.
Nutritional supplements
Omega-3 fish oil is a supplement that may help some manage PCOS. Some people today use nutritional supplements to help control their PCOS symptoms. It’s important to remember that nutritional supplements aren’t regulated by the Food and Drug Administration (FDA) and may interfere with medications or health conditions.
Speak with a physician before taking any supplements. Researchers have some evidence that omega-3 fish oil can benefit individuals with PCOS in certain ways. Nutritional supplements claim to help with hormone regulation, insulin resistance, and inflammation associated with PCOS.
Herbal supplements
Some herbal supplements are also helpful for women with PCOS. There is research that Cinnamomum cassia might be beneficial in treating metabolic complications of PCOS. Researchers have found that Vitex agnus-castus and Cimicifuga racemosa can successfully handle irregular ovulation and resultant infertility. The FDA doesn’t regulate herbal products, which can interact with drugs or health conditions.
Adaptogen herbs
When your body can not regulate insulin, it may Build up in your body and cause higher levels of male sex hormones known as androgens. Adaptogen herbs claim to assist your body in balancing these hormones. Some adaptogen herbs also claim to alleviate other symptoms of PCOS, like irregular intervals. Use caution and talk to your doctor before taking any herbal supplement, as the FDA has not evaluated their claims.
– Ashwagandha: Ashwagandha is also known as “Indian ginseng.” It helps balance cortisol levels, which might improve the stress and symptoms of PCOS.
– Maca root: The origin of the maca plant is a traditional herb used to boost libido and fertility. Maca root might help balance hormones and lower cortisol levels. It might also help treat depression, a sign of PCOS.
– Holy basil: Holy basil, too known as tulsi, addresses chemical and metabolic stress. It’s known as the “queen of herbs.” Holy basil can help decrease blood sugar, prevent weight gain, and decrease cortisol levels.
– Licorice root: The root of the licorice plant comprises A chemical known as glycyrrhizin, which has several unique properties. Licorice root was suggested as an anti-inflammatory agent. It helps metabolize sugar and balance hormones.
– Tribulus Terrestris has been revealed to help stimulate ovulation and support healthy menstruation. It might also reduce the number of ovarian cysts.
7. Probiotics
Probiotics do not just help with your digestion and gut health. They can play a significant part in treating PCOS. They can also decrease inflammation and modulate sex hormones. Probiotic foods like kimchi and supplements can help. Recently, people have started to focus a lot on the trillions of bacteria that reside in the intestines.
Scientists have now linked alterations in the gut environment, or microbiome, with many ailments, such as obesity, cardiovascular disease, and diabetes.
Researchers have discovered that these alterations might even affect sex hormones, suggesting that the microbiome may play a part in developing PCOS. Research in rats has revealed that probiotic supplements helped reverse symptoms of PCOS. Doctors consider it safe for humans to take probiotics.
Get good sleep
Sleep can affect your stress levels and helps to regulate cortisol to balance your hormones. Sleep disturbances are common for those with PCOS. Try to sleep at a regular bedtime routine and get eight hours each night. Reduce stress before bedtime by doing some yoga or listening to relaxing music. Reducing stress can regulate cortisol. Walking out and creating space for comfort and self-care may also reduce stress.
Summary
PCOS is a complex syndrome. While there’s no cure, many traditional and alternative treatments can handle the symptoms and other complications. Infertility may result from irregular ovulation and menstruation that stems from PCOS. When ovulation happens occasionally, it can be tricky to identify the fertile window when an individual can conceive. Having a normal period can help. There’s a possibility that each pure method mentioned above will help regulate menstruation. It’s important to talk with your health experts about strategies for conception and to be able to make certain that all of their concerns are addressed.