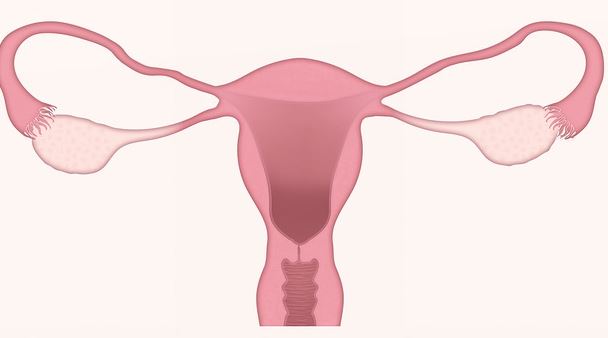
What causes PCOS?
It’s estimated that 5 to 10% of U.S. women of childbearing age have PCOS. That is roughly 5 million women, making the condition among the most common hormonal endocrine disorders among women of reproductive age. However, according to the PCOS Foundation, less than half of all women with PCOS are now diagnosed properly, meaning that millions of women are unaware of their situation.
Women with PCOS have a hormonal imbalance as well as metabolism conditions that may impact their health. The problem is especially common among women of reproductive age and may include symptoms such as excess hair growth, irregular menstrual cycle, acne, and weight reduction. While the cause of PCOS is not understood, several factors including a combination of genetic and environmental factors are widely thought to play a role.
Androgens, or male hormones, control the evolution of male traits. While all women produce small quantities of androgens, those with PCOS have more androgens than normal, which may prevent ovulation and make it difficult to have regular menstrual cycles,
The follicles grow and develop fluid, but the eggs don’t get released. Ovulation doesn’t happen, and the follicles may become cysts. If this occurs, your body may fail to produce the hormone progesterone, which is required to keep your cycle routine.
Women with PCOS also create excess estrogen or female hormones. While this does not bring about the symptoms above, long term unopposed estrogen can result in some build-up of the lining of the uterus that’s a significant risk factor for uterine cancer.
Some scientists believe that another hormone — insulin — may play a role in the body’s increased androgen production. Many women with PCOS have insulin resistance. This is quite common in women that have an unhealthy diet and exercise habits, are overweight or obese, or have a family history of type-2 diabetes.
Women whose mothers and sisters have PCOS are more likely to be affected by this condition, also.
Unfortunately, there isn’t any cure for PCOS, but overweight and obese women can help balance their hormone levels by losing weight. Otherwise, treatment is directed at managing symptoms.
A broad variety of treatment choices can help prevent any possible issues. Lifestyle changes, such as healthy eating and regular exercise, enhance the way your body uses insulin and, therefore, regulates your hormone levels improved.
It’s true that lots of women who have PCOS are overweight or obese. And it’s also a fact that obesity may make PCOS symptoms worse. However, PCOS doesn’t discriminate and can affect women of all sizes and shapes. The connection between weight and PCOS has to do with the body’s inability to use insulin properly, which may result in weight gain.
PCOS Hormonal Dysfunctions
A women’s second important and essential hormone is progesterone, which is also a companion of estrogen. Wherever estradiol functions in women’s bodies (bone, brain, breasts, uterus, skin, and everywhere), progesterone is also operating. Women have two reproductive hormones–estrogen and progesterone, whereas men just have one (testosterone).
Many women with PCOS realize they have significant hormonal dysfunctions, manifesting in many ways, such as menstrual irregularities, thyroid issues, insulin resistance, and glucose dysregulation, weight loss resistance, sleep problems, and infertility.
Among the many hormones that could be dysfunctional is progesterone. In actuality, women with PCOS do have severe fertility ” issues.” The concerns involving progesterone could lead to a higher risk for PMS and mood swings, miscarriages, pregnancy complications and preterm delivery, irregular cycles, and also significantly increased risk for uterine lining (endometrial) overgrowth (hyperplasia) and uterine cancer.
The increased uterine (endometrial) cancer risk arises from irregular and infrequent ovulation and progesterone receptor resistance. The continuous estrogen production leads to an imbalanced situation in which there is chronic, the unopposed vulnerability of the uterine lining to estrogen, without the consequences of progesterone. The progesterone receptor resistance difficulty compounds the problem by not letting the progesterone that’s created to have the desired consequences upon the adrenal glands throughout the body. The effects of estrogen dominate by not correctly changing the receptors in the uterine lining.
Progesterone for PCOS
Some have wondered whether adding progesterone cream in their PCOS treatment regimen is logical. Perhaps this could lower their risk for endometrial (uterine) cancer? Can such hormone usage help proper sleep, and enhance mood and fertility? There are progesterone products that could be easily purchased over the counter (OTC), with no medical supervision. Can a woman with PCOS get and use them? The answer is yes to using fertility but only after consultation with your doctor.
Progesterone’s biological effects are determined by the dose, the duration of the stimulation, and the existence, levels, and function of other hormones. The woman’s age may play a role. The application of fertility as a therapeutic modality is complicated and should not be undertaken without medical supervision. The prescription should be individualized so far as its dose and should be formulated by a pharmacy. Also, the goals involved with its use should be delineated, and the woman working with the progesterone must be carefully followed and monitored. Based on the individual’s particular needs and situation, other hormones may be indicated to be prescribed as well.
The world today is full of toxins, and some act as endocrine mimics or so-called endocrine disruptors. Such ubiquitous substances play further havoc with our endocrine systems, creating individualized needs and responses. This variability adds yet another layer of complexity, which must be regarded as therapies that are intended. Frequently a weekly detox program is justified. It must always be remembered that progesterone is a significant and powerful hormone with several effects throughout the body.
How does progesterone help PCOS?
How Progesterone Helps Women With PCOS
Progesterone is made by the ovaries when ovulation (release of an egg) occurs. The adrenal glands also create smaller amounts of progesterone. Progesterone and estrogen, the main female hormone, have a delicate and intricate relationship. But progesterone does the exact reverse of what estrogen does. Progesterone is very important for the woman to conceive as it prepares her body for pregnancy and regulates her monthly period.
In PCOS, the hormonal balance of the female body is missing. And because the ovaries don’t release eggs or discharge them, the progesterone levels are low. This result could be due to estrogen dominance, vulnerability to environmental imitates, insulin resistance, and many more. So while progesterone levels stay low in PCOS patients, the amount of estrogen and male hormones increase.
Therefore, it makes sense to boost progesterone levels once the body needs it the most, in the latter part of the menstrual cycle. If this is achieved, periods will get routine and can also enhance the odds of getting pregnant.
Progesterone therapy side effects
Progesterone Side Effects
Progesterone is given to women with PCOS in the kind of two chemicals — naturally-derived progesterone and artificially synthesized progestogen (or progestin). “Natural” progesterone is made of diosgenin, a chemical found in a particular sort of wild yam that grows in Mexico and from soybeans. Diosgenin is changed chemically in the lab to produce progesterone. Progestogens are chemically and structurally similar to natural progesterone and can bind to progesterone receptors and reveal an activity like progesterone.
Side effects of progesterone will be based on the sort of compound you’re taking. Side effects of natural progesterone are dose-dependent. You may feel side effects if you use a greater than the recommended dose.
Side effects of elevated progesterone levels include:
Mood swings
Acne
Oily skin
Urinary infections
Weight gain
Side effects of synthetic progestin contain:
Cardiovascular complications
Blood clots
breast and breast cancers
Insomnia
Irregular periods
Depression
Fluid retention
Liver problems
Headaches or migraines
Progesterone pill vs. cream
Progesterone pill or cream?
A progesterone or progestin cream applied in the vagina has a better prospect of being readily absorbed and be made available to the cells which need it the most. Many progestin compounds are available as tablets. When you take a progestin pill, only 10 percent of the active chemical reaches the target cells. This means that you need to ingest a lot more progestin than your body requires. Also, when this consumed progestin enters your liver, more than 30 unique metabolic by-products are made. All of these can have undesirable side effects.
Progesterone safety & precautions
Is Progesterone Safe?
Contrary to common belief, “sex” hormones act on several cells in the body. That is because the cells in those cells have complementary receptors for these hormones. Long-term progestin therapy can adversely affect the brain. National Institutes of Health (NIH) reports are to be considered, progestin treatment for PCOS may lower your chances of becoming pregnant. Research at NIH demonstrates that women treated with progestin were four times less likely to conceive.
Progesterone Safety And Precautions
Tell your doctor if you’re allergic to progesterone or any sort of progestin. Also, inform your doctor if you have some other types of allergies. Inform your doctor if you’re taking any other prescription medication, herbal supplements, or intend to take them later. You should take caution when beginning progesterone/progestin therapy if you have had any of the following medical conditions:
Unexplained vaginal bleeding between periods
Cancer of breasts or another female organ
Seizures
Migraines
Asthma
Diabetes
Stroke
Depression
Vision issues
Infection of the heart, liver, kidney or gallbladder
Tell your doctor if you’re pregnant, plan to get pregnant, or are breastfeeding. If you get pregnant during the treatment, call your physician. Progesterone may cause you to get dizzy and drowsy. Do not drive a vehicle or work on any heavy machinery until you get comfortable with all the therapy effects on your own body.
Summary
If you are suffering from PCOS, find a skilled and caring physician to work with you, carefully measure your hormone levels and inflammation markers, and look at your entire medical picture. Thankfully, through lifestyle changes, detoxification, and nutraceutical use, one’s inherent hormones can frequently be improved, which might thankfully negate the need for prescription hormones. If that goal is not achievable, you must use only quality, commercially prescribed or compounded progesterone, rather than an OTC product, comprising unknown ingredients, and without a physician’s supervision.
PCOS therapy involves a holistic approach that includes diet and lifestyle. Progesterone therapy is a little part of the approach. If you just take this hormone and dismiss diet and lifestyle changes, you’ll be sorely disappointed. Bear in mind that your body has a natural way of producing and utilizing hormones. If you’re introducing hormones, your body will react in many different ways that may not be useful for you. Symptomatic treatment of PCOS isn’t the way to manage this complex condition. The only solution to manage it is to understand the underlying cause and attack at the origin. Holistic therapies can be effective without the side-effects that come together with the drugs prescribed for PCOD administration.