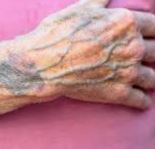
What are varicose veins?
Varicose veins are twisted and enlarged veins. Any superficial vein can become varicose, but the veins most commonly affected are those in your legs. That’s because walking and standing upright increases the pressure in the veins of the body.
For a lot of people, varicose veins and spider veins (a common, mild variant of varicose veins) are only a cosmetic concern. For some others, varicose veins can also cause aching pain and discomfort. There are times when varicose veins may contribute to more severe problems. Treatment may involve corrective steps or procedures by your doctor to close or remove veins.
Varicose veins grow when small valves within your veins stop working correctly. In healthy veins, you will find a set of little valves that are open and close to allow the blood to flow easily to the heart in one direction. If these valves become damaged or weakened, the blood flows backward, causing the veins to become swollen and enlarged.
Numerous things can cause varicose veins, such as age, weight, long periods of sitting or standing, genetics, pregnancy, being female, etc. How can you care for your varicose veins at home and how to keep them in the long run?
See: A Homoeopathic Cardiotonic Digitalis Purpurea For Heart Disease
Varicose Veins Symptoms
Varicose Veins or Spider Veins Symptoms
Varicose veins may not cause any pain. Signs you might have varicose veins include:
– Veins which are blue or dark purple
– Veins that seem twisted and bulging like cords in your legs.
– When debilitating symptoms and signs occur, they might include:
– Throbbing, burning, muscle cramping and swelling in your lower legs
– An achy and heavy feeling in your legs
– Spider veins are located closer to the skin’s surface and are often red or blue.
– Spider veins occur on the thighs, but may also be found on the face. They vary in size and frequently seem like a spider’s web.
– Itching near one or more of your veins
– Worsened pain that occurs after sitting or standing for a long time
– Spider veins are smaller than varicose veins but similar. Skin discoloration around a varicose vein
When to see a doctor: Self-care, like exercise, elevating your legs, or wearing compression stockings — helps you relieve the pain of varicose veins and might keep them from becoming worse. But if you are worried about how your veins look and feel and self-care measures have not stopped your condition from becoming worse, see your physician.
Varicose veins causes & risk factors
What causes varicose veins?
There could be one or more reasons
– Weak or damaged valves may result in varicose veins. Arteries transport blood from your heart to the rest of your cells. Veins return the blood from your body to your heart. The blood can then again be recirculated. To return the blood back to your heart, the veins on your legs must work hard against gravity.
– Muscle contractions in your legs act as pumps, and elastic vein walls help blood circulation to your heart. Your veins have tiny valves that open as blood flow toward your heart, and then shut to prevent blood from flowing backward. If these valves become weak or are damaged, blood may flow backward and rush back in the vein. This backflow causes the veins to twist or stretch.
Varicose Veins Risk Factors:
Some of the following factors can increase your risk of developing varicose veins:
– Age. The danger of varicose veins increases with age. Aging can cause wear and tear on in your veins and valves, which help regulate blood circulation. Finally, that wear causes the valves allowing some blood to flow back into your veins where it collects rather than flowing to your heart.
– Gender. Women are more likely to develop the problem. Hormonal changes during pregnancy, pre-menstruation, or menopause might be a variable because female hormones often relax vein walls. Hormone treatments (e.g., birth control pills) may increase your risk of varicose veins.
– Pregnancy. While pregnant, the quantity of blood in the body increases. This change supports the developing fetus, but can also create an unfortunate side effect — enlarged veins on your legs. Hormonal changes during pregnancy can also play a role.
– Standing or sitting for extended amounts of time. Your blood does not flow as well if you are in the same position for extended periods.
– Family history. If other family members had varicose veins, there is a higher chance you will too.
– Obesity. Being overweight puts additional pressure on your veins.
Varicose veins natural treatments
Nature has provided many options to control varicose veins.
– Olive oil: Increasing blood flow is essential when it comes to treating varicose veins. Olive oil has anti-inflammatory, toning, and calming properties that will decrease the size of dilated and enlarged veins and activate blood circulation after being absorbed through the skin. Olive oil contains a high content of essential fatty acids, vitamin E, and minerals. The high content of Omega-3 fatty acids boosts the passing of blood through the veins and restores the use of the unidirectional valves.
– Garlic: Garlic is used for several conditions that are linked to the heart and the circulatory system. Garlic produces allicin and ajoene, which can be sulfurous compounds having the ability to boost blood circulation. They contribute to the avoidance of inflamed blood vessels and into the prevention of blood clots. Garlic has very potent anti-inflammatory properties that are excellent for reducing the swelling of varicose veins and the discomfort they can cause. Additionally, garlic contains quercetin, a flavonoid that can help strengthen the veins and blood vessels, preventing them from suffering any harm.
– Rose oil: Rose essential oil is created by extracting Rosa Damascena, and researchers have uncovered it comprises several therapeutic chemicals known to promote healing within the body. It improves blood flow, inhibits blood pressure, and strengthens blood vessels. It’s an effective essential oil for leg veins. By ensuring that the blood vessels remain healthy and unclogged, future occurrences of varicose veins will be avoided.
– Lemons: Lemons are high in vitamin A, C, B6, E, thiamin, riboflavin, folate, niacin, pantothenic acid, magnesium, copper, calcium, iron, potassium, zinc, phosphorus, and protein. The high vitamin C helps protect cells from harmful free radicals and protect against oxidative damage. Furthermore, it helps avoid varicose veins, high blood pressure, and skin wrinkling according to research done by the American Society of Clinical Nutrition.
– Cayenne pepper: Cayenne pepper is considered a miracle cure for varicose veins. It contains vitamin C and bioflavonoids (an antioxidant that’s used to treat allergies, viruses, or arthritis, and other inflammatory conditions). It can also help reduce atherosclerosis, promotes fibrinolytic activity, and prevents variables that result in the formation of blood clots, all of which may help reduce and cure varicose veins.
– Cabbage: Cabbage is packed with antioxidants and phytochemicals. It is also full of insoluble fiber, beta-carotene vitamins – B1, B6, K, E, and C, and lots of minerals such as magnesium, potassium, calcium, iron, and sulfur. When these phytochemicals and antioxidants touch the affected area, they hit the veins through the pores to help the blood clot and stop the seepage of blood.
– Apple cider vinegar: Apple cider vinegar contains high levels of enzymes, protein, and bacteria that are friendly. However, the main component in apple cider vinegar is acetic acid that can kill harmful bacteria or stop it from multiplying. Moreover, many animal studies have proven that vinegar can lower blood glucose, blood pressure, blood clots, and cholesterol.
– Aloe vera: Aloe vera gel contains salicylic acid and antiseptic compounds that kill off the germs that cause acne that makes it a terrific natural remedy for breakouts and an exceptional cleanser for the skin. It’s also packaged with minerals, antioxidants, enzymes, and vitamins A, C, and E, that all work together to fortify the skin’s barrier.
– Carrots: Carrots are a good source of vitamins and minerals, particularly vitamin A (from beta-carotene), potassium, biotin, vitamin K (phylloquinone)sulfur, and vitamin B6. They help in fixing skin tissue in the event of damage. It may penetrate the skin and assist it with recovering faster from outside wounds and injury.
– Tomato seeds: Tomato seeds contain salicylic acid with properties similar to aspirin and function as an anticoagulant for improving blood circulation and preventing blood clots. Additionally, tomatoes are full of lycopene, which focuses primarily on our cell membranes and prevents damage to our own cells’ lipids. When applied to the skin topically, it reduces the veins’ appearance, and it affects the depth, strength, and fluidity of our membranes, enabling nutrients to be absorbed and preventing toxins from entering.
– Witch hazel: Witch hazel has its medicinal properties in the tannins, essential oils, choline, flavonoids, and saponins. Its properties make it quite effective in treating skin disorders of all kinds, including psoriasis and eczema. Pharmacological studies at the University of Michigan indicate that witch hazel strengthens veins and functions as an anti-inflammatory. Tannins provide witch hazel’s astringent action, which helps tighten distended veins and fix their regular structure. This process helps shrink tissue and act as mild sedatives to ease the pain and discomfort associated with varicose veins.
– Horse chestnut seed: Horse chestnut extract is an effective remedy for free radicals. Horse chestnut seeds are used for a long time to heal varicose veins due to their anti-swelling and anti-inflammatory properties. Horse chestnut seed is full of quercetin and kaempferol glycosides, two powerful antioxidants with extreme disease-fighting capabilities. Regular use of horse chestnut extract can cure chronic venous insufficiency. This benefit is because the infusion of the horse chestnut seeds is believed to prevent the breakdown of proteins inside the capillary walls.
– Marigold: Marigold, (otherwise called calendula) is an anti-inflammatory and can fight inflammation and infections. It contains flavonoids, triterpene, saponins, and carotenoids that are considered to act in numerous ways. This effect can include increasing venous tone, improving lymphatic drainage, and reducing capillary hyperpermeability. It can be taken as a drink or applied topically as an ointment to bring down swelling, ease pain, and prevent inflammation. Additionally, it has soothing and firming properties after being absorbed through the skin, decreasing the size of dilated veins, and triggering blood circulation in the affected regions. Massaging this as an ointment to the skin relieves pain and will stimulate the functions of the lymphatic system. This will enable the best elimination of these toxins from varicose veins.
– Parsley: Parsley is full of thiamin, riboflavin, niacin, vitamins A, K, C, and E, vitamin B6, vitamin B12, calcium, iron, pantothenic acid, choline, folates, magnesium, manganese, phosphorus, potassium, zinc, and copper. Besides, it contains several flavonoid antioxidants that protect the cells from free radical damage responsible for blood-related issues. Parsley is abundant in vitamin C also contains potent collagen producing properties. It’s also absorbed by the skin’s pores quite easily and helps reduce the appearance of scars and blemishes that make it a perfect home remedy for preventing and treating varicose veins.
How to prevent varicose veins?
How can you prevent varicose veins naturally?
– An anti-inflammatory diet: An anti-inflammatory diet will help reverse inflammation and enhance blood flow to your veins. The healthy flow will make it feasible to heal varicose veins quicker and prevent future ones from forming. A diet rich in sugars, fats, caffeine, processed foods, and alcohol will cause arterial damage, blood pressure issues, and lower the flow. However, a diet full of copper, bioflavonoids, fruits full of antioxidants and tannins, and water can help prevent varicose veins.
– Exercise: Exercise often to improve your leg circulation, leg strength, and vein strength. Focus on physical activity that works your legs, like walking or jogging. This can enhance the appearance of varicose veins and block the formation of new ones. Exercise shouldn’t be overly strenuous and should be immediately stopped if there is any pain or distress.
– No standing or sitting in one place for a long time: Standing or sitting for a long time in one place makes it harder for the blood to go to the leg veins against gravity. Because of this, the pressure on your veins increases, and this may lead to damage to the valves of your veins. Moving around even only a little bit every half an hour will reduce the strain and improve your blood flow.
– Healthy weight: Individuals that are overweight are more prone to develop varicose veins, particularly obese women and the elderly. This added risk is due to carrying excess body weight puts higher levels of pressure in your veins. Increased pressure could lead to harm in the valves and finally result in varicose veins. Trying to maintain a healthy weight may also force us to eat healthily and exercise regularly. This way, we’ll have the ability to easily notice abnormalities within our bodies and treat them in time.
– Essential oils: Various essential oils are incredibly beneficial in improving blood flow while also reducing inflammation and hormonal imbalances. Some of the finest essential oils for preventing and treating varicose veins include: cypress essential oil, German chamomile, lemon oil, rose oil, olive oil, vitamin E oil, and evening primrose. Heal the oil of your choice in your legs or the place your varicose veins start to show several times each day. Moreover, consider using essential oils on your skin as often as possible after a shower to get smooth skin and overall well-being.
– No high heels: High heels alter the natural walking movement, shifting the weight to the forefoot and feet and leads to the calf muscles to stay contracted. This contraction causes the pooling of venous blood in the leg. After the foot is raised from the ground, the foot veins fill with blood. As the arch and heel of the foot contact the ground, the blood flows to the relaxed calf veins. The calf muscles then contract, which divides blood up into the deep veins and can cause varicose veins.