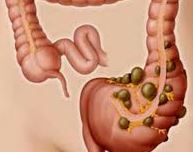
What is Ulcerative Colitis?
Ulcerative Colitis (UC) is a condition that involves inflammation and ulceration of the lining of the large intestine, medically called the colon. (Colitis= inflammation of colon) The digestive system is a system of organs responsible for digesting the food we eat so that nutrients in the food are available to the body to provide the required energy. The digestive system consists of a long tube, which connects the mouth to the anus. Once food leaves the mouth, it enters the part of the GI tract called the esophagus and then the stomach. In the stomach, food pauses for some time and is mixed up with acid and juices present in the stomach. It then passes into the small intestine, which measures about 20 feet in length. The small intestine has three parts; the part nearest the stomach is the duodenum, the next part is the jejunum, and the third part that connects to the large intestine is the ileum. The small intestine is the site where most of the food is digested with the assistance of secretions from the liver, gallbladder, and pancreas. The nutrients from this digested food are then absorbed through the small intestine.
Followed by the small intestine is the large intestine, which is more frequently referred to as the colon. The large intestine (colon) is 6-7 feet in length. The first part of the colon is called the caecum, and the appendix is found there. The caecum and appendix are situated in the right lower portion of the abdomen. The large intestine then extends upward (this portion being called as ascending colon), then takes a turn and passes across (portion called as the transverse colon) and then goes downwards (descending colon). At the end of the descending colon exists a portion of the large intestine (the sigmoid colon) that opens into the rectum. The colon’s main function is to absorb water from the processed food residue that arrives after the nutrients have been absorbed in the small intestine. The last part of the colon is the rectum, which is a reservoir for feces. Feces are stored here until a bowel movement occurs.
Ulcerative Colitis causes
Inside the large intestine, the inflammation of the inner lining (mucosa) causes the death of the colon lining cells, and this results in sores or ulcers. Also, the inflammation makes the colon frequently empty, resulting in diarrhea. As the lining of the colon is destroyed, ulcers form releasing mucus, pus, and blood.
– Ulcerative Colitis Causes
The precise cause of this terrible affliction is still unknown. Theories about what causes ulcerative colitis abound, but none have been proven. The current studies suggest that there is more than one factor responsible for the development, maintenance, and relapse of Ulcerative colitis. The causes may involve but are not limited to, heredity, genetic factors, environmental factors, or disturbances of the immune system.
One of the major underlying causes is abnormal activation of the immune system, which leads to ulcerations in the intestines. For easy understanding, we will divide these factors into two groups i.e., extrinsic and intrinsic factors.
– Extrinsic factors:
Diet
Intake of junk food and low-residue high-refined sugar has been correlated in many studies with susceptibility to having ulcerative colitis. Many sufferers of ulcerative colitis notice flare-up of the problem following specific food.
Infections: Some researchers feel that ulcerative colitis may be related to certain infections digestive caused by microorganism E. Coli. One theory holds that modern measles virus, improperly cleared from the body, results in low grade, chronic inflammation of the intestinal lining.
Drugs: The studies have also shown links between intake of oral contraceptive pills and Ulcerative colitis. May patients experience a flare-up of the condition following modern medicine drugs like antibiotics and NSAIDs. Isotretinoin, a commonly used drug for severe acne, is found to trigger UC and Crohn’s disease in some patients.
– Intrinsic factors:
Disturbance of the immune system: Some experts believe that there may be a defect in one’s immune system responsible for ongoing inflammation in the intestinal wall. The disturbance is thought to be either of two.
Allergy: Some studies suggest that Ulcerative colitis is a form of an exaggerated allergic response to a certain food or to the presence of some microorganisms present in the intestine.
Autoimmunity: Autoimmunity simply means an allergy to oneself. Most recent research indicates that ulcerative colitis can be a form of autoimmune disease in which the body’s defense system starts attacking its own organs and tissues. One amongst them is a large intestine.
Genetics: Current research suggests that certain genetic factors may increase the likelihood of a person having Ulcerative colitis.
Hereditary factors: If your immediate family members have ulcerative colitis, then your chances of having the disease increases.
Psychosomatic: The mind plays a vital role in maintaining a healthy or diseased condition of the body. The medical community has accepted that any kind of emotional stress has a definite detrimental effect on the immune system and can be the root cause of chronic diseases like ulcerative colitis. In fact, it is a very common experience of physicians that many patients mention that their problem of Ulcerative colitis started after some stressful situations in life, or their problem gets worse following stressful events.
Ulcerative Colitis symptoms
Symptoms of Ulcerative Colitis
Ulcerative colitis affects each individual uniquely. Some suffer only mild symptoms, but others have severe and disabling symptoms with frequent flare-ups. Usually, the symptoms tend to come and go, and there may be long periods without symptoms. Usually, however, the symptoms reappear after an interval, which varies from days to months or even years. Although all the ulcerative colitis sufferers may not have all the symptoms of the disease, the common and consistent ones are as follows:
– Diarrhea: The most common symptom of UC is diarrhea. When severe, it may require frequent visits to a toilet (in some cases up to 20 or more times a day). The disorder typically begins gradually, with crampy abdominal pain and diarrhea that is usually bloody.
– Blood in the stools: UC is characterized by the presence of blood in the stools. Blood is admixed with the stools and not in the form of blood clots. Passage of blood clots usually suggests some other diagnosis or condition. In addition to blood, stools may also contain mucus and pus.
– Tenesmus: Inflammation of the gut can affect the nerves in such a way as to make the patient feel that there is a stool present ready to be evacuated when there is not. That results in the symptom known as tenesmus, where there is a painful urge to defecate, but nothing comes out.
– Nausea, vomiting, and abdominal pain or cramps: Flare-ups of ulcerative colitis may be associated with nausea, vomiting, abdominal cramps, and diarrhea. Abdominal pain may not be a consistent feature of UC. When pain is present, it may indicate severe inflammation or the development of a complication such as an abscess or a perforation of the intestinal wall.
– Fever, fatigue, loss of appetite are usual accompaniments with consequent weight loss. The patient may become weak and very sick.
– Constipation: At times, some UC patients experience constipation during periods of active disease.
– Loss of water and nutrients: With increased diarrhea, the person may lose invaluable water and nutrients from the body and may present with dry mouth, sunken eyes, a fast heartbeat, and pale skin.
A flare-up is a stage when the rectum and/or colon become inflamed. During a flare-up, people experience periods of increased symptoms of ulcerative colitis, such as bloody diarrhea, rectal bleeding, abdominal pain or cramping, and an urgent need to go to the bathroom. Flare-ups can vary in duration and intensity.
Remission is the time between flare-ups of ulcerative colitis when people experience few, mild, or no symptoms. Periods of remission vary in duration, anywhere from a matter of days to many years.
Ulcerative Colitis types
Types of Ulcerative Colitis:
The inflammation related to ulcerative colitis usually occurs in the rectum and lower part of the colon, but it may affect the entire colon. Ulcerative colitis rarely affects the small intestine except for the lower section, called the ileum. Depending upon which portion of the intestine is most affected by UC, it is put under various types as follows.
– Inflammation of Entire colon =Pan-colitis (pan =entire, colitis=inflammation of colon)
– Rectum= Proctitis
– Sigmoid colon (S-shaped portion of colon located just above the rectum) = Sigmoiditis
– Beyond sigmoid colon= Left-sided colitis
See: Home remedies for gas & bloating pain
Natural treatments for Ulcerative Colitis
There are many natural treatment possibilities for people wanting to manage UC.
– Herbal medicines: A 2019 review emphasized several herbal substances that may reduce UC symptoms. These included Andrographis paniculata infusion, Plantago ovata seeds, aloe vera gel, wheatgrass juice, and Boswellia serrata gum resin.
In the review, the authors indicate that specific compounds in these herbal remedies encourage immune activity and supply antioxidants that reduce inflammation. The researchers recommend that individuals with UC should just use them as supplementary remedies alongside traditional medicines.
– Probiotics: Eating foods that contain probiotics, such as yogurt, may help handle UC.
Probiotics are bacteria or germs that promote the growth of healthy bacteria in the digestive tract. Some foods, like kimchi and yogurt, contain natural probiotics. Alternatively, someone could buy probiotics over the counter at most major food stores and drugstores. A 2019 research looked at how individuals with UC responded to using probiotics. Researchers found that 57 percent of people who used the probiotics reported a positive overall experience. Also, 50 percent of the responders noted an improvement in their symptoms, such as stool frequency and feel. Individuals that are interested in probiotics should speak with a healthcare professional who can recommend reputable supplement brands.
– Lifestyle changes: Sometimes, someone with UC may realize that making simple lifestyle changes supplies some symptom relief. These changes could be beneficial:
– group therapy to help with the psychological ramifications of UC
– exercise, which may support weight control and boost energy levels
– Dietary changes: Particular dietary changes can make a difference in helping people reduce symptoms and flare-ups. These may include:
– drinking lots of water to stop dehydration, especially during a bout of nausea
– drinking electrolyte beverages, which can help a person keep an electrolyte equilibrium when nausea could lead to dehydration
– eating well and avoiding restrictive diets
– Calcium and vitamin D supplements, as many people with UC don’t consume enough of these nutrients
– eating many smaller meals instead of three big ones
– reducing fatty, buttery foods intake
– eating a low-fiber diet
– avoiding milk products, as many people with UC have lactose intolerance
Some people may discover that keeping a food journal can be helpful. By recording their food intake and symptoms, someone could work out which foods trigger flare-ups and eliminate them from their diet.
There’s not any specific research supporting a particular diet program for UC. However, some research suggests that certain chemical plant chemicals known as phytochemicals can help alleviate symptoms of UC.
In 2014, a review of research found that phytochemicals from apples, cocoa, green tea, along with other foods and nutritional supplements, could decrease UC symptoms in animals. However, the review suggests a need for additional studies to ascertain the benefits of these compounds in humans.
– Conventional UC treatments: Some traditional treatments can send UC into remission. Herbal remedies work best alongside more conventional treatments, which individuals with UC generally tolerate well despite them having some side effects. Drugs and therapies carry a risk of side effects. Someone should speak with their doctor about possible side effects when they get a prescription for new medicine.
Summary
Someone may have the ability to alleviate their symptoms by using some natural remedies alongside conventional treatments. Making dietary adjustments, Ayurveda, acupuncture, taking probiotics, and exercising can help. However, you should always take medication based on their physician’s instructions. If someone experiences any unwanted side effects from drugs, they ought to speak to their doctor about their symptoms.